This website uses cookies to ensure you get the best experience on our website.
- Table of Contents
and ELISA kits, proteins related to Atopic Dermatitis.
Atopic dermatitis, commonly known as eczema, is a chronic inflammatory skin condition characterized by intense itching, redness, and dry patches of skin. This condition affects millions worldwide and can significantly impact quality of life. While it frequently begins in childhood, atopic dermatitis can persist or even start in adulthood. The exact cause of atopic dermatitis remains uncertain, but it is believed to involve a combination of genetic, environmental, and immune system factors. Living with this condition means managing flare-ups and seeking treatments that alleviate symptoms. Current research is pivotal, focusing on understanding the underlying mechanisms of the disease and the immune system responses involved. This knowledge is crucial for developing targeted therapies. Antibodies, especially those designed to interact specifically with immune pathways integral to atopic dermatitis, represent a promising frontier in this research. These studies not only aim to improve treatment efficacy but also enhance the lives of those affected by atopic dermatitis.
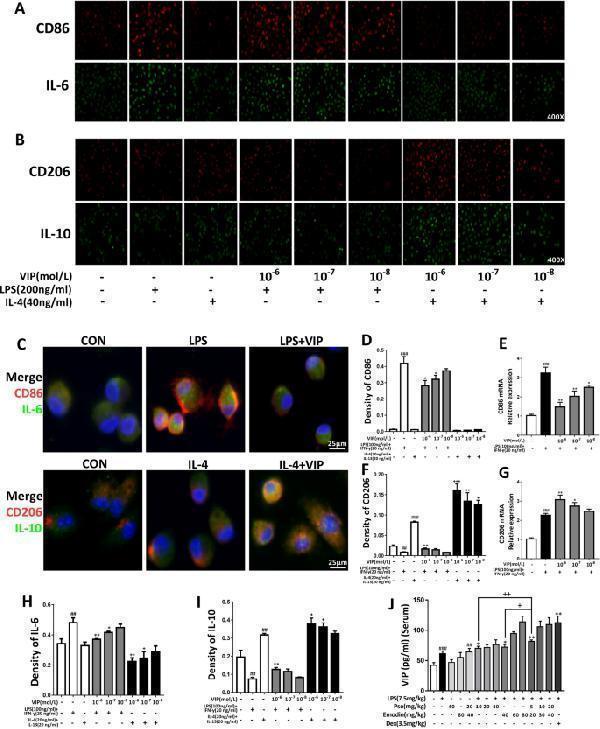
Anti-IL10 Antibody, VIP inhibited (M1) macrophage and activated (M2) macrophage in LPS + IFN-γ‐induced or IL-4 + IL-13-induced AMs. Effects of Pseudoephedrine + emod...
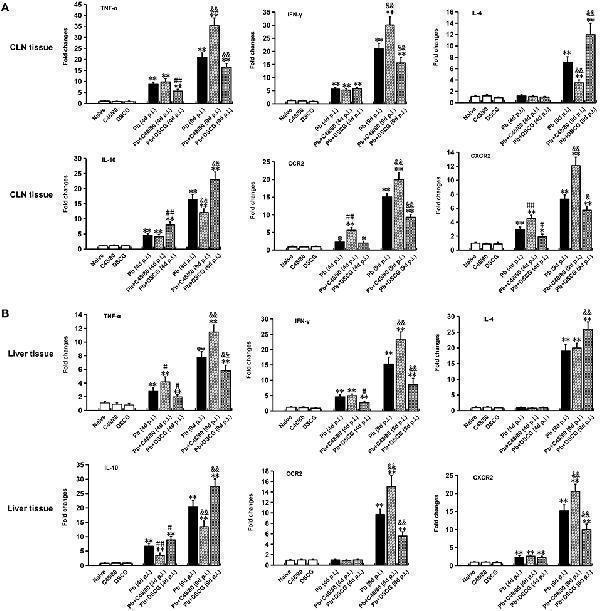
Anti-GRO alpha/Cxcl1 Antibody Picoband®, Cytokine and chemokine receptor mRNA expressions in CLN or skin from PbANKA-infected mice with C48/80 or DSCG treatment using qPCR m...

Anti-Interferon gamma/IFNG Antibody Picoband®, Western blot analysis of IFNG using anti-IFNG antibody (A00393-3).
Electrophoresis was performed on a 5-20% SDS-PAGE gel at 7...
| Protein Name | Gene Name | Function |
|---|---|---|
| Filaggrin | FLG | Plays a critical role in the formation of the skin barrier, mutations lead to skin barrier dysfunction. |
| Interleukin-4 | IL4 | Key cytokine in the initiation and maintenance of the Th2 response, involved in B cell differentiation. |
| Interleukin-13 | IL13 | Regulates inflammatory responses, involved in IgE synthesis and airway hyperresponsiveness. |
| Interleukin-31 | IL31 | Contributes to pruritus sensation and dermatitis. |
| Thymic Stromal Lymphopoietin | TSLP | Initiates Th2 mediated inflammation, implicated in airway inflammation and dermatitis. |
| Ovalbumin specific IgE | IGHE | Marker of allergic reaction, involved in atopic sensitization. |
| Eotaxin-3 | CCL26 | Chemokine that recruits eosinophils, involved in inflammatory responses. |
| Periostin | POSTN | Enhances Th2 cytokine response, associated with allergic inflammation. |
| Thymus and Activation-Regulated Chemokine | CCL17 | Attracts Th2 cells, involved in the development of atopic diseases. |
| Interleukin-5 | IL5 | Promotes eosinophil production and function, important for allergic airway inflammation. |
| Interleukin-22 | IL22 | Induces epidermal hyperplasia and dermal inflammation. |
| Interleukin-33 | IL33 | Induces Th2 cytokine production, plays a pivotal role in atopic dermatitis. |
| Keratinocyte-derived chemokine | CXCL1 | Chemokine involved in neutrophil recruitment and activation. |
| Interleukin-12 | IL12B | Induces Th1 type immune response and suppresses Th2 type immune responses. |
| Interferon gamma | IFNG | Critical for innate and adaptive immunity against viral and intracellular bacterial infections and for tumor control. |
| Toll-like receptor 2 | TLR2 | Plays a crucial role in the innate immune response to microbial agents. |
| Interleukin-10 | IL10 | Anti-inflammatory cytokine, important in restricting immune responses to pathogens. |
| Regulatory T cells | FOXP3 | Crucial for maintaining immune tolerance, prevents autoimmune disease. |
One crucial sub-research area in atopic dermatitis (AD) is immune dysregulation. AD is often characterized by a complex interplay of immune system abnormalities, including both innate and adaptive immune responses. The disorder features a predominant type 2 helper T-cell (Th2) profile which actively participates in the inflammatory processes of the skin. These Th2 cells release specific cytokines, such as interleukin-4 (IL-4), interleukin-13 (IL-13), and interleukin-31 (IL-31), which contribute to both the inflammation and the characteristic itch seen in AD. Moreover, recent research has begun to explore the role of other immune cells like the Th22 and Th17 cells and their cytokines in the pathology of AD. Understanding the dysregulated immune pathways in AD is critical for developing targeted therapies that can more effectively manage or potentially alter the course of the disease, aiming to offer relief from the chronic symptoms that define this condition.
Another pivotal sub-research area in atopic dermatitis revolves around skin barrier dysfunction. The protective barrier of the skin, primarily made up of cells and lipids, is essential in maintaining hydration and protecting against environmental factors, including allergens and microbes. In AD, genetic factors, such as mutations in the gene coding for filaggrin—a protein vital for maintaining skin barrier integrity—are commonly observed. These mutations lead to a compromised skin barrier, which allows increased transepidermal water loss and lowers the threshold for irritants and allergens to penetrate the skin. This contributes to the initiation and exacerbation of the inflammatory processes. Research in this domain focuses not only on understanding the molecular basis of barrier dysfunction but also on developing interventions that can enhance barrier function and thus improve disease outcomes. This area is crucial because effective restoration of barrier function can significantly reduce disease severity, improve patient quality of life, and decrease reliance on pharmacological interventions that might have more significant side effects.