This website uses cookies to ensure you get the best experience on our website.
- Table of Contents
How the Immune System Builds Its Defense
Antibody diversity allows the immune system to generate millions of unique antibodies, many of which can be developed through specialized antibody discovery and antibody generation services, each capable of targeting
Affinity gauges the binding strength of a single bond, while avidity measures the combined stability of multivalent interactions. Understanding the difference enhances assay design, vaccine evaluation, and therapeutic efficacy.
Affinity vs avidity describes how tightly antibody attach to antigens, and together, these values predict real-world performance. High-affinity IgG molecules often show a low dissociation rate constants (Kd) below 10⁻⁹ M, yet even weaker binding sites can yield strong avidity when arranged on a pentameric IgM. Roughly 80% of early infection tests rely on avidity principles, whereas most monoclonal antibodies undergo affinity maturation before approval, a process supported by our antibody production services. This reflects a fundamental aspect of molecular interactions essential in diagnostics, drug development, and biomedical research.
A single antigen-antibody reaction can decide whether a pathogen infects a cell membrane or is cleared from it. Strong binding reduces the likelihood of escape, enhances diagnostic sensitivity, and can prolong drug residence time. Therefore, scientists track both affinity—the force at a single binding site—and avidity—the collective force from immune complexes formed by multiple bonds.

Fig.1 Illustrating antigen-antibody interaction, comparing affinity and avidity. Shows a monovalent antibody binding to a single epitope (affinity) alongside a multivalent antibody binding to multiple epitopes on a pathogen surface (avidity).
Affinity is the attraction between one antigen-binding site and one epitope. It reflects how quickly the complex forms (association rate constant)and how slowly it breaks apart (dissociation rate constant). Strong affinity implies a low Kd, often 10⁻⁹ M or lower for mature IgG. Small mutations in complementarity-determining regions can shift affinity by a thousand-fold due to changes in hydrogen bonds and hydrophobic interactions at the binding interface.
Researchers choose different tools depending on throughput and sensitivity:
High-affinity antibodies improve assay specificity because weak binders wash away during stringent steps in Western blotting or ELISA.
Avidity combines multiple affinities. An IgM pentamer, with ten identical Fab fragments, can latch onto a multivalent antigen structure even if each site binds weakly. Cooperative binding stabilizes complexes, especially when antigens display repeating epitopes. This process integrates Bond Strength with structural arrangement to resist dissociation.
Laboratories often use an avidity ELISA in which samples bound to the antigen are washed with a chaotropic agent, such as 6 M urea. The avidity index equals the signal retained after treatment divided by the signal before treatment, expressed as a %.
Clinicians apply this in diagnosing rubella, toxoplasmosis, and other infections, differentiating acute from past exposure in the humoral immune response.
Affinity and avidity describe related but distinct aspects of molecular binding, and understanding their differences is essential for interpreting experimental results.
| Factor | Affinity | Avidity |
|---|---|---|
| Definition | Strength of a single binding site | Combined strength of multiple sites |
| Unit | Dissociation rate constant (Kd) | Avidity index or functional strength |
| Influenced by | Amino-acid contacts, shape fit | Valency, epitope density, flexibility |
| Main role | Determines specificity | Enhances binding stability |
| Primary assay | SPR, BLI, equilibrium ELISA | Avidity ELISA, functional tests |
These practical examples show how affinity and avidity influence diagnostic accuracy, therapeutic design, and vaccine assessment in real-world applications.
Rapid tests for early infection often detect IgM because its high avidity yields visible agglutination. For confirmation, labs switch to IgG affinity tests that discriminate true positives from antibody cross reactivity and false signals.
Drug developers raise affinity through mutagenesis and selection cycles. Values below 10⁻¹¹ M increase target occupancy at lower doses. In contrast, bispecific antibodies sometimes leverage avidity, arranging two weaker arms to reduce off-target effects while maintaining strong overall attachment, an approach enabled by custom monoclonal antibodies.
This process considers antibody concentration, functional affinity, and how each antibody molecule binds and remains stable within antibody-antigen complexes.
After vaccination, affinity matures through somatic hypermutation, and avidity rises as antibodies switch from IgM to IgG. Monitoring the avidity index helps researchers predict the durability of protection and decide whether booster shots are necessary.
Selecting the appropriate assay depends on the research objective. When detailed binding kinetics are required, techniques such as Surface plasmon resonance (SPR) or bio-layer interferometry (BLI) provide real-time measurements of the association rate constant and dissociation rate constant. For high-throughput screening of multiple antibody clones, equilibrium ELISA is often the first step, with promising candidates later validated by SPR for precise affinity data. In infectious disease studies, avidity ELISAs that incorporate chaotropic washes help distinguish recent infections from long-term immunity by analyzing the stability of antigen–antibody complexes. For mucosal immunity, IgA assays are essential, as secretory IgA exhibits unique resistance to enzymatic digestion, offering insights into protective responses at epithelial barriers.
Affinity and avidity together describe how antibodies interact with antigens, guiding numerous decisions in diagnostics, research, and medicine. Focusing solely on one value can be misleading; a balanced evaluation ensures accurate conclusions and successful product development.

Are you looking to refine your assays, develop high-performance antibodies, or showcase new findings?
Submit an inquiry to connect with our expert team. Discover how tailored assay design, collaborative research, and exhibition opportunities can enhance your projects and foster new partnerships.
Roughly 10% of people worldwide live with an autoimmune condition, and more than 80 of these disorders trace at least part of their pathology to antibodies that have turned on the body. These rogue molecules—often referred to as autoantibodies—trigger inflammation, degrade healthy tis
Antibodies, also known as immunoglobulins, are specialized proteins produced by the immune system to identify and neutralize foreign invaders such as bacteria, viruses, and toxins. Their ability to recognize and bind to specific antigens make them play a critical role in the immune response and serve as key tools in biomedical research, including advanced applications like...
Antibody types form the foundation of adaptive immune system. In humans, IgG alone accounts for approximately 75% of circulating antibodies, while the other four classes—IgM antibodies, IgA, IgE, and IgD—fill specialized roles in blood, tissues, and secretions. Together, these Y-shaped glycoproteins create a flexible defense network that identifies, neutralizes, and clears pathogens with remarkable precision.
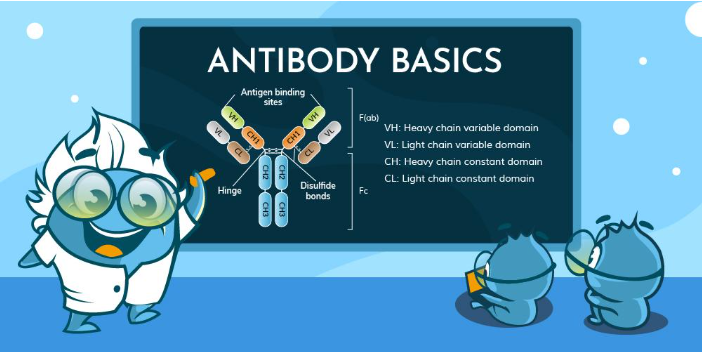
All antibodies share a common heterotetrametric structure consisting of heavy and lights connected by disulfide bonds in the hinge regions but variations in their constant regions define each antibody isotype. Understanding these differences is critical for selecting the right reagents for immunodiagnostic tests, designing effective vaccines, and developing therapeutic monoclonal antibodies. Each type plays a specific role in the adaptive immune response, inf...
The immune system is a complex network that protects the body from harmful pathogens such as bacteria, viruses, and other foreign substances. Central to this defense mechanism are various molecular components, including antibodies, antigens, epitopes, haptens, and immunogens. Each of these components plays a unique role in the immune response, and understanding their differences is crucial for comprehending how the immune system functions.
Antibodies, also known as immunoglobulins, are specialized Y-shaped proteins produced by B cells, a type of white blood cell. These proteins are critical in the immune response as they identify and neutralize foreign objects like bacteria and viruses. The structure of antibodies allows them to specifically recognize and bind to antigens, effectively marking them for destruction by other immune cells. In research applications, this specificity can be enhanced or visualized through chemical labeling—a process typically facilitated by an antibody conjugation service. This specificity is due to the unique binding sites on the antibody that match specific parts of the antigen, known as epitopes.
As antibody research moves from basic immune recognition to reagent and therapeutic development, researchers may generate binders through approaches such as single B cell antibody discovery or phage display library screening, depending on whether the goal is to preserve native heavy/light chain pairing or to run fully in vitro, high-throughput selection.
Antigens are molecules or molecular structures, often found on the surface of pathogens, that can elicit an immune response. They are typically proteins or polysaccharides and are recognized by the immune system as foreign. The interaction between antigens and antibodies is highly specific, akin to a lock and key, where the antibody binds to the antigen to neutralize or flag it for removal. This interaction is fundamental to the body’s ability to recognize and remember pathogens, forming the basis of immunity.
Epitopes, also known as antigenic determinants, are specific regions on an antigen that are recognized by antibodies. Each antigen can have multiple epitopes, allowing for the binding of different antibodies. This multiplicity enables a robust and versatile immune response, as various antibodies can target different parts of a single pathogen. The specificity of epitopes is crucial in vaccine development, as vaccines aim to introduce harmless forms of epitopes to stimulate an immune response without causing disease.
Haptens are small molecules that, by themselves, are not immunogenic, meaning they cannot independently provoke an immune response. However, when haptens bind to larger carrier proteins, they form a complex that the immune system recognizes as foreign, triggering an immune response. This phenomenon is particularly important in pharmacology and allergen studies, where certain drugs or small molecules can act as haptens, causing allergic reactions when they bind to proteins in the body.
Immunogens are a subset of antigens that can trigger an immune response on their own. While all immunogens are antigens, not all antigens qualify as immunogens. For instance, a hapten is an antigen but not an immunogen unless it is attached to a carrier protein. Immunogens must have certain properties, such as adequate size and molecular complexity, to effectively stimulate the immune system. This distinction is important in vaccine development and allergy research, where understanding what makes an antigen immunogenic can inform treatment strategies.
Depending on the downstream application, antibodies raised against these immune targets may later be reformatted for different production systems. For example, smaller binding formats such as Fab, scFv, or VHH are often well suited to microbial expression systems for antibody fragment production, especially when Fc-mediated functions or mammalian glycosylation are not required.
We’ve provided a table below that summarizes and highlights the distinct roles and interactions of these immune system components.
| Term | Description | Example |
|---|---|---|
| Antibody | Y-shaped proteins produced by B cells that specifically recognize and bind to antigens, aiding in the neutralization and destruction of pathogens. | IgG, IgM, IgA |
| Antigen | Substances, often proteins or polysaccharides on the surface of pathogens, that trigger the production of antibodies and stimulate an immune response. | Viral proteins, bacterial cell wall components |
| Epitope | Specific regions on antigens that are recognized and bound by antibodies. | Binding site on a viral protein |
| Hapten | Small molecules that are not immunogenic on their own but can elicit an immune response when bound to a larger carrier protein. | Penicillin, certain drugs |
| Immunogen | A type of antigen capable of independently provoking an immune response, possessing the necessary properties to stimulate immune cells. | Whole viruses, bacterial toxins |
The immune system's effectiveness hinges on interactions among antibodies, antigens, haptens, epitopes, and immunogens. Antibodies recognize and bind to antigens, identifying foreign molecules for destruction. Haptens, though non-immunogenic alone, provoke responses when linked to larger proteins. Epitopes are specific antigen regions targeted by antibodies, while immunogens independently trigger immune responses. Comprehending these dynamics not only advances immunological understanding but also...
The purpose of using a secondary antibody is to amplify the primary antibody and antigen interactions. Before choosing a secondary antibody for your experiment, ask yourself the following 3 questions to help you choose the appropriate one:
The secondary antibody should be raised against the host in which the primary antibody was raised. For example, if the primary antibody was raised in rabbit, you will need an anti-rabbit secondary antibody raised in a species other than rabbit.
The secondary antibody has to be directed specifically against the isotype of the primary antibody. For example, the polyclonal primary antibodies are generally of the IgG isotype and thus the corresponding (species specific) secondary antibody needs be an anti-IgG antibody. The monoclonal